How do the US and European lipid guidelines compare? See commentary from the EAS here
Tools for integrating risk factors and imaging
The MESA website has some useful online tools for estimating arterial age and age and sex percentile calcium scores. Check them out here.
The UK's NICE committee has also produced a PDF that explains the concept of using calcium scoring in subjects with chest pain of recent onset.
Lifetime cardiovascular risk (as opposed to 10 year risk) is another approach, suggested by Berry and colleagues in the NEJM.
A lifetime risk calculator can be found here - QRisk website.
Useful tool from the Confirm CT registry that integrates coronary CTa findings with clinical risk factors and demographic data - Confirm Tool.
Who is most at risk of heart disease?
Abridged from Dr Arthur Agatston writing at the Huffington Post:
Who is more likely to die from a heart attack or other cardiovascular-related event?
A. A person who is overweight, has high cholesterol, high blood pressure, and diabetes, and a calcium score of 0?
or
B. A person with no risk factors and a calcium score of over 400?
This is important to be aware of, since nearly 1 million American men and women have a heart attack every year.
The answer is B. Strikingly, it is estimated that nearly 50 percent of those who suffer fatal heart attacks don't even know they have risk factors.
Recently, a large and important study has found that even if you don't have any of the conventional risk factors for heart disease -- high blood pressure, high cholesterol, family history, prediabetes and diabetes, smoking, being overweight, high triglycerides, a sedentary lifestyle -- it doesn't necessarily mean you're home free.
The study, which was published in the journal Circulation Cardiovascular Imaging, looked at more than 44,000 individuals free of known coronary heart disease. Each person underwent a noninvasive computed tomography (CT) scan of the heart for coronary calcium and was then followed for a median of 5 years for whether or not they died of any cause.
Those with no coronary calcium and no risk factors had the lowest death rate, whereas those with a calcium score of over 400 and three risk factors had the highest death rate. Not surprising.
What's notable about this study, however, is that the individuals with no risk factors and a calcium score of more than 400 (people who are not generally candidates for aggressive prevention) had substantially higher death rates compared with individuals with three risk factors and the absence of coronary calcium (approximately 17 vs. approximately 3 per 1,000 person-years).
The authors also noted that nearly half of the individuals meeting eligibility for statin therapy based on Justification for the Use of Statins in Prevention: an Intervention Trial Evaluating Rosuvastatin (JUPITER) criteria had no CAC and experienced an extremely low event rate, with an unfavorable estimated number needed to treat for 5 years of 549 to prevent 1 CHD event compared with 42 among those with the presence of CAC.
What does this striking data mean? It suggests that people with coronary calcium (with and without other risk factors) are more likely to die, and that a selected group of patients without risk factors might benefit from further risk assessment and preventive therapies.
Atherosclerosis in abdominal aorta may predict adverse cardiovascular events
Interesting study from the University of Texas, using MRI to screen for atherosclerosis.
Accumulation of plaque tells us there is increased risk for peripheral vascular occlusion, stroke, and abdominal aortic aneurysms, but not all forms of cardiovascular events, including heart attacks and death from cardiovascular disease,“ he said. ”In contrast, thickening of the aortic walls is more likely to be predictive of all forms of cardiovascular disease.
This is a different approach to merely screening for risk factors of atherosclerosis, and one that is endorsed by SHAPE.
Risk factor control or drug therapy in lowering cardiovascular deaths
I'm not sure exactly how this intriguing graph was constructed, but it demonstrates that nearly half of the reduction in CHD deaths over the past 50 years is due to new therapies, whilst most of the remainder stems from better risk factor control.
From the ESC Guidelines
Another approach to understanding the changes in CVD mortality and incidence rates is by applying models such as the IMPACT mortality model. Based on information on changes in coronary risk factors and in treatment as obtained from the results of RCTs regarding the effectiveness of different treatment modalities, it estimates the expected influence on CHD mortality by age and gender. This model has been applied in different countries; the results from these studies are rather consistent and similar to what has been observed in other studies of the same subject, as summarised in Figure 1. Beneficial reductions in major risk factors—in particular smoking, BP, and cholesterol—accounted for more than half of the decrease in CHD deaths, although they were counteracted by an increase in the prevalence of obesity and type 2 diabetes; 40% of the decline in CHD death rates is attributed to better treatments of acute myocardial infarction, heart failure, and other cardiac conditions. Results from clinical trials and natural experiments also show that a decline in CHD mortality can happen rapidly after individual or population-wide changes in diet or smoking.

Percentage of the decrease in deaths from coronary heart disease attributed to treatments and risk factor changes in different populations (adapted from Di Chiara et al. Does surveillance impact on cardiovascular prevention? Eur Heart J 2009;30:1027–1029.)
Imaging of progression of carotid atherosclerosis - case unproven
A study I recently read in the Lancet reports results of an individual patient data meta-analysis, which show that cIMT progression is not associated with incident myocardial infarction, stroke, or vascular death in the general population (hazard ratio 0·98, 95% CI 0·95–1·01, adjusted for age, sex, mean common carotid artery intima-media thickness, and vascular risk factors).
A single measure of carotid IMT may be useful for predicting risk in asymptomatic intermediate risk adults, although far less so than calcium scoring by CT according to the most recent guidelines.

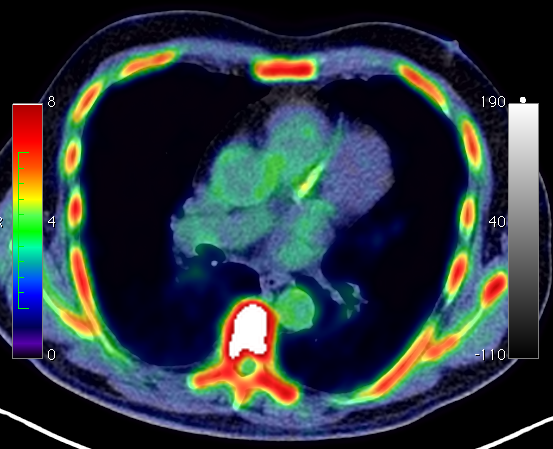
Coronary artery PET imaging with NaF - the debate continues
The paper we published in JACC with colleagues in Edinburgh continues to be discussed. A letter and our reply were recently aired on the JACC website.
It’s certainly true that we don’t fully understand the dynamics of NaF uptake into coronary atherosclerosis. And we are still working on ex-vivo experiments to determine the binding characteristics of the tracer in atherosclerosis, which will likely be similar to that expressed in bone tissue. We do know that the degree of NaF uptake correlates with cardiovascular risk, and there is only a weak relationship between NaF and FDG uptake. So it is likely telling us something different from metabolic activity of the plaque.
Whether it is predictive of future cardiovascular events, can be altered with therapy or is reproducible - time (and lots of research efforts) will tell.
Risk prediction in hypertrophic cardiomyopathy
Excellent webcast of an ESC 2012 presentation by Perry Elliot of the Heart Hospital. He's an expert in HCM. He covers the prediction of risk in that disease using genetic, clinical and imaging factors. He mentions the ESC and ACC guidelines and the development of a new web-based tool for refining risk on an individual patient basis.
Can three minutes of exercise a week help make you fit?
From the BBC website:
A few relatively short bursts of intense exercise, amounting to only a few minutes a week, can deliver many of the health and fitness benefits of hours of conventional exercise, according to new research, says Dr Michael Mosley. But how much benefit you get from either may well depend on your genes.
This seems unbelievable to me. But there is some limited data to back up the claims.
For a fuller explanation and some fascinating videos of the technique in action, checkout the Horizon broadcast (only for UK viewers I suspect).
Physical exercise and vascular risk
From Circulation, the Physical Activity and Inflammatory Markers Over 10 Years: Follow-Up in Men and Women from the Whitehall II Cohort Study
Background—Inflammatory processes are putative mechanisms underlying the cardio-protective effects of physical activity. An inverse association between physical activity and inflammation has been demonstrated but no long-term prospective data are available. We therefore examined the association between physical activity and inflammatory markers over a 10-year follow-up period.
Methods and Results—Participants were 4289 men and women (mean age 49.2 years) from the Whitehall II cohort study. Self-reported physical activity and inflammatory markers (serum high-sensitivity C-reactive protein [CRP] and interleukin-6 [IL-6]) were measured at baseline (1991) and follow-up (2002). Forty-nine percent of the participants adhered to standard physical activity recommendations for cardiovascular health (2.5 hours per week moderate to vigorous physical activity) across all assessments. Physically active participants at baseline had lower CRP and IL6 levels and this difference remained stable over time. In comparison to participants that rarely adhered to physical activity guidelines over the 10 years follow-up, the high adherence group displayed lower logeCRP (β=-0.07, 95% CI, -0.12, -0.02) and logeIL-6 (β=-0.07, 95% CI, -0.10, -0.03) at follow up after adjustment for a range of covariates. Compared to participants that remained stable, those that reported an increase in physical activity of at least 2.5 hours/wk displayed lower loge CRP (B coefficient =-0.05, 95% CI, -0.10, -0.001) and loge IL-6 (B coefficient =-0.06, 95% CI, -0.09, -0.03) at follow up.
Conclusions—Regular physical activity is associated with lower markers of inflammation over 10 years of follow-up and thus may be important in preventing the pro-inflammatory state seen with ageing.
Keep running. The only way out is through.